Modernisation of Medication Management Systems in Hospitals in Ireland
Written by Dr Diana Hogan-Murphy, Medication Safety Pharmacist, University Hospital Galway
Electronic medication management systems inclusive of electronic prescribing and advanced pharmacy software and robotic systems have been shown to improve patient safety, workflow and cost efficiencies, and governance by increasing traceability and enhancing accountability.
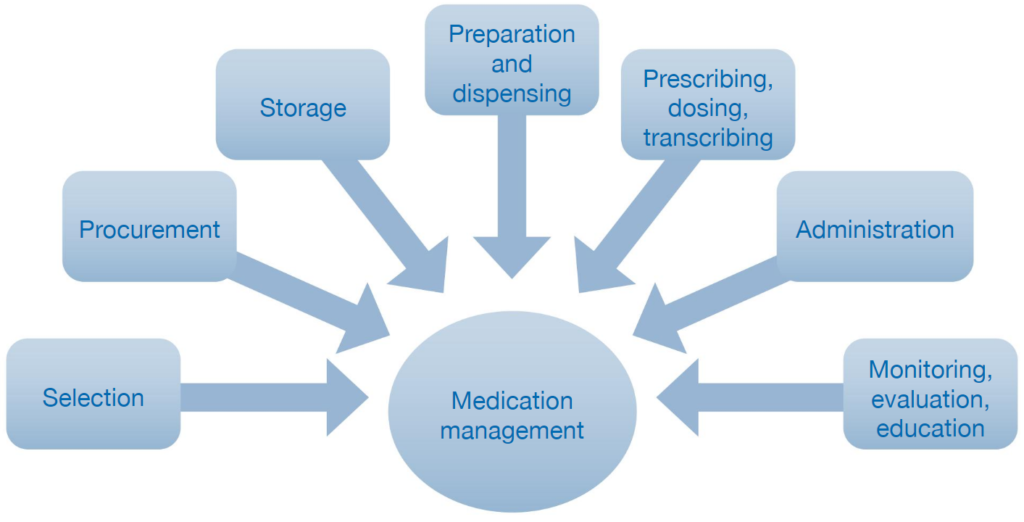
Medication management in hospitals is complex. It incorporates the entire process of how medicines are selected, procured, delivered, prescribed, administered. This is as well as reviewed to achieve informed and desired patient outcomes. At the forefront of medication management is medication safety. Therefore, it is an important and topical issue that has been highlighted by the World Health Organization and various national organisations.
 Whilst the use of medicines is currently increasing in number and complexity which requires more decision-making capability and potentially amplifies medication error risks, medication management systems in Irish hospitals have remained largely paper-based and unchanged over the last few decades. It is estimated that three million medication errors occur in hospitals in Ireland per annum. However, estimating the true incidence of medication-related errors can be problematic. This is due to the various definitions and technologies which is lower than peer countries which spend up to three per cent of their healthcare budget on health technologies.
Whilst the use of medicines is currently increasing in number and complexity which requires more decision-making capability and potentially amplifies medication error risks, medication management systems in Irish hospitals have remained largely paper-based and unchanged over the last few decades. It is estimated that three million medication errors occur in hospitals in Ireland per annum. However, estimating the true incidence of medication-related errors can be problematic. This is due to the various definitions and technologies which is lower than peer countries which spend up to three per cent of their healthcare budget on health technologies.
Emphasis on patient safety, defined as the prevention of errors and adverse effects to patients associated with healthcare. It is placed on a system of care delivery that prevents errors, learns from errors that do occur. It is built on a culture of safety that involves healthcare professionals, organisations, and patients. Electronic medication management systems inclusive of electronic prescribing and advanced pharmacy software and robotic systems have been shown to improve patient safety, workflow and cost efficiencies, and governance by increasing traceability and enhancing accountability. These systems represent a technical development. But also represents a mindset, a method of thinking, an attitude, and a commitment to improve healthcare. Successful reform and delivery is highly dependent on realising the potential of these systems as a change catalyst.
As well as assessing and fostering readiness for system implementation, fundamentals required to modernise processes include sufficient funding; a hospital formulary; skilled staff in adequate numbers; good, safe, usable, reliable, interoperable, readily available, and value for money hardware and software; testing at scale; clinical champions; organisational support; a multidisciplinary implementation team; contingency plans; comprehensive staff training; in addition to ongoing evaluations.

A modernisation of the hospital pharmacist career structure is equally required. There is a strong desire among the hospital pharmacy community to improve patient safety, quality of service, and service efficiency. Pharmacists are experts in medication management. They are integral to the successful deployment of these systems. Pharmacists in addition to this, play a pivotal role in supporting acute clinical care pathways.
However, we are a small professional group within the broader hospital context and underrepresented when compared to wider hospital strategies. The current disparity in the level of the clinical pharmacy provision within hospitals risks system implementation. Without structures that can take the lead on all aspects of medication management and assurances that pharmacy is represented at senior levels to ensure medication management related projects are expert led within all hospitals, the large investment required for modernising current systems will be at risk.
Electronic medication management systems should be viewed by all stakeholders as a positive practice shift towards process optimisation and healthcare quality effectiveness. Therefore, we can learn from others as the late runners into this space to ensure we achieve the best balance of features, safety, usability, and value. The vision is not for duplication of current systems but for innovation which will map future successes of system adoption and improve patient safety and efficiency.
Key drivers of system implementation:
- Implementation of the Hospital Pharmacy Review/Career Structure agreement
- Developing, communicating, and maintaining strong management support throughout the organisation and identifying champions, preferably senior prescribers and recognised specialist pharmacists
- Estimating necessary financial resources such as hardware, software, additional human resources, training, and technical support with an emphasis on patient safety benefits and efficiencies to justify financing
- Fostering a culture of change by placing value on the system and promoting and supporting implementation highlighting benefits to both system users and patients
- Adequate, timely, and ongoing on-site training as well as technical support with protected time for training
- Reconfiguring roles, responsibilities, and work tasks
- Assessing and managing unrealistic expectations and concerns pre-implementation with clear goals and anticipated benefits
- Ensuring system backup as well as considering workflow design as part of the implementation process
- Developing formal goals, objectives, as well as key indicators of success
- Anticipating challenges in the implementation process
If you would like to receive an HPN magazine every month, complete the form below to be added to the mailing list. Only those who meet the expected criteria for readership will be added to the list. SUBSCRIBE
Follow us:

